Archive for June, 2013|Monthly archive page
PWD w/ PE – Part 2
Okay, so apparently ending the last post with “to be continued” may have caused some undue panic…but to those of you that reached out to make sure I was okay, thank you. You’re a kind bunch. And just to clarify, I’m not dying…at least not at a substantially faster rate than I was before.
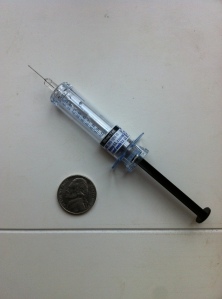
So back to the story…after reviewing the CT test results and considering the fact that I’d been walking around with this for 2 weeks, my doctor thankfully decided that admitting me to the hospital wasn’t really necessary. After all, all they would do is put me on blood thinners and then I’d sit around waiting for it to work. I was started on 2 different types of medication (fun fact, btw, “blood thinners” are more accurately anticoagulants…they don’t really thin the blood, just reduce the ability to clot). I was started on 1 Coumadin pill (easy enough to swallow), and twice daily injections of Lovenox. Since I’ve been injecting things for, oh…21 years or so, my doctor figured I could handle this on my own. And I can, but that doesn’t stop it from hurting like hell. For you diabetic folk out there, it’s basically like giving yourself a Glucagon injection twice a day. Here’s a shot (get it?) of that friendly needle:
It’s been 9 days so far and we’re still getting the dosage worked out (up to 3 pills a day now), so I’m becoming good friends with the folks in the lab at my doctor’s office. Apparently I’ve become a bit of minor celebrity around there…one test they ran on me to check for all sorts of genetic clotting disorders required 13 test tubes of blood…when I came in the next day and only had to do 1 tube, I made a comment to the nurse about the previous day’s test and she said “oh, I heard about you!”. Oh, and the insides of my elbows now look like Lance Armstrong before the Tour de France a heroin addict’s, so there’s that.
Unfortunately, we still don’t know where the clots came from, and my doctor seems to think we may never exactly figure it out. I don’t have any of the common genetic or biological clotting issues, and all of the ultrasounds and other scans have come up empty. Unlike pretty much everything else, this isn’t even one of those “more likely to happen in people with diabetes” things. Right now the leading contender is a clot that somehow formed due to severe dehydration after the stomach virus I had a month or so ago.
Thankfully at least as far as diabetes is concerned, things have gone pretty smoothy. The medication doesn’t appear to be affecting my blood sugar (although the lack of exercise isn’t helping things), and aside from taking longer to stop bleeding from the numerous holes I’m poking in myself daily, things are going pretty well. That’s not to say I haven’t tried to find answers to diabetes & PE questions online, but finding information on those 2 conditions in combination is a bit like hunting Captain Ahab’s white whale.
My medical team has been great though. I’m not saying getting a potentially fatal condition is the best route for everyone to take, but it does seem to get you better than average treatment from the healthcare community…I got a direct call on my cell from my endo on the day of the diagnosis, and my PCP has actually come out to the waiting room several times to talk to me while I was there for lab work. I’d gladly trade “the star treatment” to be healthy, but it is nice to feel that they’re concerned.
So that’s pretty much where we stand now. We know what’s wrong, but we don’t know why, and we don’t know exactly when it will be better, but we’re working on it. It sounds like eventually I’ll be back to 100% with no permanent issues, but I know it’ll take longer than I want it to. In the meantime, thanks for reading and I appreciate the support. Talk to you soon!
PWD w/ PE – Part 1
(soon, that rather letter-thrifty blog title will make sense)
About 3 weeks ago, something went wrong inside me. I first suspected something was awry when I was on a relatively easy-paced bike ride with a work friend, and had to stop after about 5 miles because it felt like my heart was going to beat out of my chest. I couldn’t seem to catch my breath, even when coasting downhill. I think if my life were an episode of House, this would be the point where the “camera” swoops down my throat and centers in on the internal malady. Since I don’t have that luxury, I assumed this all stemmed from the fact that I had forgotten to take my asthma inhaler that day. Granted, it seemed a little severe for missing one dose, but I thought that combined with Spring allergies was certainly to blame. Over the following week, I resumed my normal medication, but the problem didn’t go away. I’d try to go for a run, and couldn’t make it more than half a mile before I was forced to stop, gasping for air. Even just going up the stairs in our house made me winded and made my heart race. I haven’t been training as hard since the marathon, but I wasn’t THAT out of shape.
At the beginning of last week, I finally called my doctor as the problem wasn’t getting any better. Of course it was several days before I could get an appointment, but I finally got in last Thursday. I explained my symptoms to my doctor, still assuming that I just needed an adjustment in asthma medication or something simple like that. We went through all the normal breathing exam stuff…listening to my lungs, pulmonary function test, and so on. The doctor came back and said something to the effect of “you have impressive lung capacity, but there’s nothing wrong with your asthma”. Good news for my fitness self-esteem, I guess, but not so helpful for a diagnosis. There was a noticeable shift in my doctor’s demeanor at this time. We went from “let’s get you something to clear this up” to “we don’t know what’s wrong with you”. In my experience, it’s rarely a good thing when they don’t know what’s wrong with you. Next they ran an EKG, to see if there was anything unusual with my heart activity. The EKG results weren’t wildly abnormal, but they weren’t normal either. The doctor recommended that we follow up on Friday with an echocardiogram (ultrasound of the heart) to see if anything looked out of the ordinary. They also ran a battery of blood tests to try to rule out any other causes…anemia, blood clots, etc.
Friday morning, I got a call from the nurse saying that the D-dimer (clotting) test had come back slightly elevated, so they wanted to run a chest CT scan as well. I showed up for my heart echo test, and it was arranged for me to go over to the hospital for the CT scan immediately after. There were no immediate red flags from the echo, so while I guess that helped rule some things out, it didn’t get us an answer either. I had never had a CT scan before, so I didn’t really know what to expect. I honestly don’t remember a ton about it, other than the fact that the contrast dye made me feel like I was peeing on myself, just as the technician had warned. After the test, I was moved to a waiting area while the radiologist read the results. I say “waiting area”…it really felt like more of a timeout corner. It was just a chair in a little hallway next to the ice machine.
After about 10 minutes, a new face came to meet me…”Hi, I’m Dr. ____, I’m the radiologist on duty” (I’d like to say I left the name blank for anonymity, but honestly I don’t even remember). “You have multiple pulmonary embolisms…blood clots in both of your lungs. We’re going to have to admit you this afternoon. We’re trying to get in touch with your primary care doctor now…just wait here and we’ll come get you shortly.”
There was a little more conversation with the radiologist, but not a ton of elaboration on what that meant, how serious it was, and how long I’d be in the hospital. I called my wife at work and told her the news, and then sat in the “timeout corner” waiting for more instruction while hospital staff came and refilled their cups with ice and water in my little hallway.
(to be continued…I’m about to fall asleep writing, and I’m sure you’re about the same from reading.)
 Comments (1)
Comments (1)